CHANDIGARH
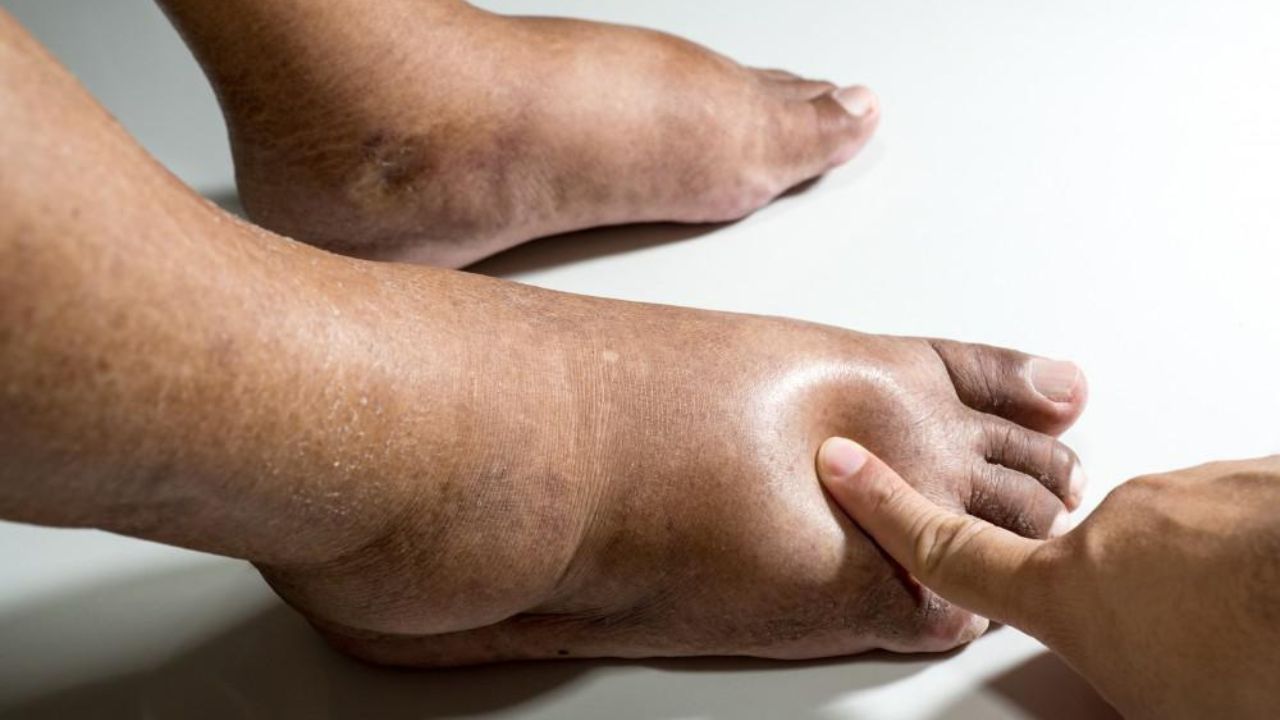
Sores that develop at the foot and stay for more than a week are now as diabetic feet. These kinds of sores are mainly seen in diabetic patients.
It starts from a minor wound and further develops into a blister, dry, cracked skin, or a recent cut or scrape.
However, unlike most other wounds, they don’t cure over a period and might spread, which could be a cause of concern somewhere. For this reason, it’s critical to get treatment for diabetic foot ulcers as soon as possible.
Diabetic feet are contracted due to many reasons which are listed below:
- Any nerve injury
- Having poor blood flow, particularly in your extremities
- Elevated blood sugar (hyperglycemia)
Risk factors for diabetic foot ulcers
All diabetics are at risk for foot ulcers, however, specific variables make diabetic foot ulcers more likely to occur. As follows:
- Diabetic nerve damage
- Ill-fitting footwear
- Improper foot care
- Ingrown toenails or improper toenail clipping
- Earlier foot ulcer history
- Coronary artery disease
Experts suggest these treatments for diabetic ulcers.
As we all know the mode of treatment depends upon the injury, and your body allows it. At first, your physician will examine the injury, clean the wound and bandage it with a sterile dressing in less serious situations.
If the case will be severe then, it may lead to surgery.
Some self-care for diabetic foot are:
- Frequently examine your foot.
- Avoid staying barefoot even at home.
- After the feet wash, clean them properly.
- Carefully clip your nails.
- Most essential, consult your doctor if you discover an injury to your feet.
Follow these Dos & Don’ts
- Eat the exact size of footwear.
- Your shoes must be covered around the toes, have a sturdy or protected sole, and a soft insole.
- Avoid wearing tight shoes since they might hurt or pinch your feet.

 हिंदी
हिंदी